Causes
of a painful neuropathy
Causes
of a predominantly sensory neuropathy
Proprioception/Vibration
loss only
Clinico-pathological
Differential Diagnosis
Axonal
sensorimotor (Most are predominantly
sensory, motor predominant in bold)
Pure
Sensory, Large Fibre, Ataxic Neuropathy
Polyneuropathy
and Optic Neuropathy
Myeloneuropathies
(Combined Myelopathy and Polyneuropathy)
Neuromyopathies
(Combined Myopathy and polyneuropathy)
Mononeuropathy (Mononeuritis)
Multiplex
Diabetic
neuropathies (see complications of DM)
Hereditary
Neuropathy with Liability to Pressure Palsy
Classification
Location
• Mononeuropathy
o Multiple mononeuropathy
• Polyneuropathy (peripheral neuropathy)
• Plexopathy
• Radiculopathy
o Polyradiculopathy
• Polyradiculoneuropathy
• Autonomic
Fiber type
• Sensory
o Small-fibre sensory (Painful neuropathies with dissociated sensory loss)
o Large –fibre sensory (Ataxic neuropathies)
o Small and large (global sensory loss)
• Motor
• Autonomic
Pathology
• Demyelinating (see below for full DDx)
• Axonal
• Neuronal
Pathological classification
|
|
Demyelinating |
Axonal |
Neuronal |
|
Pattern |
Proximal =
distal |
Distal >
proximal; length-dependent |
Non-length-dependent;
UE, LE, face |
|
Onset |
Acute/subacute |
Slow evolution |
Rapid |
|
Symptoms |
Paresthesia
and weakness |
Dysesthesias
and distal weakness |
Paresthesias,
gait ataxia |
|
Sensory signs |
Vibration and proprioception > pain and
temperature |
Pain and temperature affected > vibration and
proprioception |
Vibration and proprioception > pain and temperature |
|
Motor |
Distal and
proximal weakness |
Distal
weakness |
Proprioceptive
weakness |
|
DTRs |
Areflexia |
Distal areflexia |
Areflexia |
|
NCS |
Velocity
affected > amplitude |
Amplitudes
affected > velocity |
Sensory amplitudes
affected; radial > sural |
|
Nerve biopsy |
Demyelination and remyelination |
Axonal degeneration and regeneration |
Axonal degeneration but no regeneration |
|
Prognosis |
Rapid recovery |
Slow recovery |
Poor recovery |
|
Causes |
GBS, diphtheria, CIDP, DM, MMN |
Toxic, metabolic, HIV, CMT2, DM |
Sjögren's, cisplatin, pyridoxine |
Fibre Type Classification
|
|
Symptoms |
|
|
Small Fibre |
Diabetic Alcohol (mixed) Amyloidosis HIV (and Rx) Sjogren’s Syndrome Sarcoidosis Uraemia Leprosy Fabry disease HSAN |
Pain – para/dysesthesia Reduced pin prick and temperature
|
|
Large Fibre |
Sjogren’s Syndrome B12 Cisplatin Pyridoxine toxicity Friedreich’s ataxia |
Numbness Tingleing Poor balance Reduced vibration,
proprioception, reflexes |
|
Small and large |
Carcinomatous Diabetic (late) Hereditary |
|
|
Motor predominant |
GBS CIDP CMT Diabetic (amyotrophy) Porphyria Lead Multifocal motor neuropathy Brachial neuritis |
Cramps Twitching Reduced strength and reflexes |
|
Autonomic |
Botulism GBS Amiodarone Vincristine Amyloid DM |
Dry mouth, erectile dysf,
gastroparesis, diarrhoea, syncope Orthostasis, unequal pupils |
|
Mixed motor and sensory |
CMT Alcohol |
|
Symptom
Classification
Talley and O’Connor
Causes of a painful neuropathy
1.
DM
2.
Alcohol
3.
Vitamin B12 or B1
4.
Carcinoma
5.
Porphyria
6.
Arsenic or thallium poisoning
7.
Hereditary (most are not painful)
Causes of a predominantly sensory neuropathy
1.
Carcinoma
2.
Paraproteinaemia
3.
Vitamin B6 intoxication
4.
Sjogren’s syndrome
5.
DM
6.
Syphilis
7.
Vitamin B12 deficiency (occasionally)
8.
Idiopahtic
Proprioception/Vibration loss only
• Consider myelopathy - posterior spinal cord syndrome (Spinal Cord Disease)
• Neuroapthy – Especially DM and hypothyroidism
Pain/temperature loss only
• Consider central cord syndrome
• Syringomyelia
• Anterior spinal artery thrombosis
• Peripheral neuropathy (especially DM, amyloid, Fabry’s)
• Unilateral
o Brown sequard
o Lateral medullary syndrome
Clinical Approach
|
|
|
|
What? |
Sensory Motor Autonomic Combination |
|
Where? |
Length-dependent vs non-length dependent? Symmetry vs Asymmetrical |
|
When? |
Acute Subacute Chronic |
|
What setting? |
Medical history (DM, cancer, medications) Alcohol Family history Occupational exposures |
Burns and Mauermann (Neurology Clinical Practice 2011)
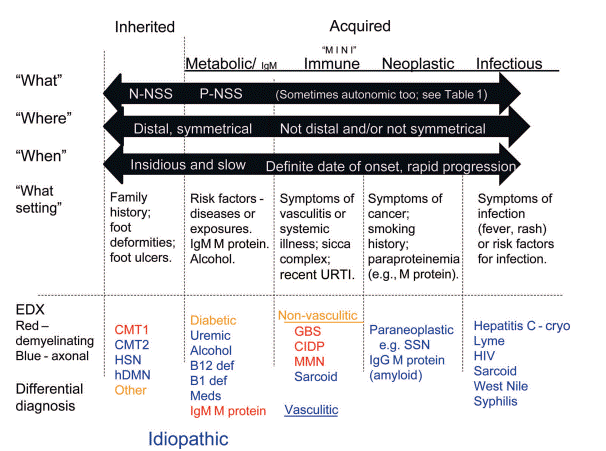
Clinico-pathological Differential Diagnosis
Clinico-pathological
Differential Diagnosis
Axonal
sensorimotor (Most are predominantly
sensory, motor predominant in bold)
Pure
Sensory, Large Fibre, Ataxic Neuropathy
Polyneuropathy
and Optic Neuropathy
Myeloneuropathies
(Combined Myelopathy and Polyneuropathy)
Neuromyopathies
(Combined Myopathy and polyneuropathy)
|
|
|
|
|
|
Axonal sensorimotor (Most
are predominantly sensory, motor predominant in bold)
|
||||
|
Full list of causes |
Common Causes |
First line tests |
Second line tests |
|
|
Chronic |
Metabolic ·
DM,
uraemia, hypothyroidism, acromegaly, hepatic failure,
hypoglycaemia/hyperinsulinaemia Nutritional ·
B12,
Folate, Thiamine, vitamin E, copper, bariatric surgery Vascular ·
Vasculitis ·
Chronic
hypoxia, polycythemia Neoplastic
(infiltrative) ·
Leukaemia/lymphoma,
Multiple myeloma, NF 1 and 2 Paraneoplastic ·
Various Infectious ·
HIV,
HTLV-1, HCV, Whipple Toxic ·
Alcohol,
Nitrous oxide Immune ·
Sjogren,
SLE, RA, scleroderma, MCTD, Coeliac, primary biliary cirrhosis,
hypereosinophic syndrome Paraprotein ·
MGUS,
amyloidosis, Waldenstrom, cryoglobulinaemia Hereditary ·
CMT2, abetalipoproteinaemia, neuroacanthocytosis, adult onset Tay-Sachs |
DM Alcohol B12 MGUS-
associated Uraemia Hypothyroidism Thiamine |
BSL, HbA1C B12 SPEP Electrolytes TSH Thiamine FBC |
CXR ANA, ENA ANCA ACE Anti-neuronal
antibodies Coeliac
serology HIV HCV Lyme serology HTLV-1 Cryoglobulins Copper Vitamin E Vitamin B6 Salivary gland
biopsy Fat pad biopsy Genetic: CMT2 testing |
|
|
|
|
|
|
Demyelinating sensorimotor
|
||||
|
|
Full list of causes |
Common Causes |
First line tests |
Second line tests |
|
Acute |
GBS Diptheria Hypophosphataemia Toxic (meds):
amiodarone, tacolimus, bortezomib, Anti-TNF-alpha GVHD Arsenic Hexane (Glue
sniffing) |
|
|
|
|
Chronic |
Inflammatory ·
CIDP ·
CIDP
associated with SLE, IBD, DM, HIV, HCV, HBV, GVHD, Anti-TNFalpha agents ·
MMN Paraprotein/haematological
disorders ·
MGUS
– IgM/anti-MAG ·
MGUS
– IgG/IgA ·
POEMS/Osteosclerotic
myeloma ·
Castleman
disease ·
Waldenstrom’s ·
Cryoglobulinaemia,
melanoma, lymphoma Hereditary/genetic ·
CMT1,
CMT4, DSD/CHN, CMTX ·
Lysosomal
leukodystrophies ·
Lipoprotein
disorders (Tangier disease) ·
Familial
amyloid ·
Cerebrotendinous
xanthomatosis ·
Cockayne
syndrome ·
Mitochondiral
disorders ·
HNPP Other ·
Severe
DM |
CIDP (and
variants) MMN HNPP CMT1 (DM) |
SPEP CSF GM1 Abs HbA1C |
HIV HBV HCV Malignancy
work-up Skeletal survey
ANA PMP22 genetic
testing Nerve biopsy |
|
|
|
|
|
|
Small Fibre
|
||||
|
|
Causes |
Common |
First line tests |
Second line tests |
|
|
Idiopathic Endocrine/Metabolic ·
B12,
Hypothyroidism, DM Infection ·
HCV ·
HIV Immune ·
Sjrogens,
SLE ·
Paraneoplastic ·
Sarcoidosis ·
Vasculitis Genetic/hereditary ·
Fabry
disease ·
Tangier
Disease ·
HSAN Paraprotein ·
MM,
cryoglobulinaemia Toxic ·
Arsenic,
thallium, nucleoside analogues, chemotherapy |
Idiopathic DM Amyloidosis Alcoholic HIV Sjrogens SLE |
BSL, HbA1C SPEP HIV serology ANA, ENA Electrolytes TSH FBC B12 |
Lipid profile Coeliac
serology ACE Paraneoplastic
(Anti-Hu) Cryoglobulins HCV Alpha-galactosidase Skin biopsy Fad-pad biopsy Salivary gland
biopsy |
Pure Sensory, Large Fibre, Ataxic Neuropathy
|
||||
|
|
Causes |
Common |
First line tests |
Second line tests |
|
Sensory
neuronopathy |
·
Sjrogens ·
Paraneoplastic ·
Idiopathic ·
Toxic:
Pyridoxine excess, cisplatin, thalidomide, linezolid, metronidazole, taxanes ·
HIV ·
EBV |
|
ANA, ENA Anti-neuronal
Ab’s Vit B6 HIV |
|
|
Demyelinating |
·
Acute: o
Ataxic
GBS o
Fisher
Syndrome o
Diptheria ·
Chronic: o
Sensory
CIDP o
Anti-MAG/IgM
MGUS o
CANOMAD o
CISP |
|
Anti-MAG SPEP Anti-Gq1b |
|
|
Misc. |
·
Tabes
dorsalis ·
Coeliac ·
HTLV-1
or 2 ·
Vitamin
B12, B1, E ·
Anti-sulfatide
antibodies |
|
Syphilis Coeliac
serology B12 Thiamine |
HTLV Vitamin E |
Motor Neuropathies
|
||||
|
|
Causes |
Common |
First line tests |
Second line tests |
|
Axonal |
Acute/subacute: ·
GBS
- AMAN ·
Porphyria ·
Toxic:
lead, dapsone, amiodarone, vincristine Chronic: ·
Distal
hereditary motor neuropathies ·
CMT2 |
|
CSF Porphyrins Heavy metals Genetic testing |
|
|
Demyelinating |
·
GBS-AIDP ·
MMN ·
CIDP ·
CMT1
and CMT 4 ·
Toxic:
amiodarone |
|
CSF Anti-GM1 Genetic testing |
|
Autonomic
|
||||
|
|
Causes |
Common |
First line tests |
Second line tests |
|
|
Acute/subacute: ·
GBS ·
Paraneoplastic ·
Autoimmune
autonomic ganglionopathy (ganglionic AchR antibodies) ·
Sonnective
tissue diseases ·
Post-viral Chronic ·
DM ·
Amyloidosis ·
Hereditary o
HSANs
Porphyria, Fabry ·
Infectious o
HIV,
leprosy, diphtheria, Chagas ·
Toxic o
Vincristine,
heavy metals, alcohol |
DM |
BSL, HbA1C |
CSF Anti-neuronal
antibodies ANA, ENA SPEP HIV Heavy metals |
Mononeuritis Multiplex
|
||||
|
Sensory and
motor Axonal |
Vasculitis Sarcoidosis Infections
(HIV, HCV, HBV, CMV) Neoplastic Coeliac Diabetes |
|
|
|
|
Sensory and motor
Demyelinating |
HNPP CIDP (MADSAM GBS/AIDP Tangier disease |
|
|
|
|
Motor
Demyelinating |
MMN |
|
|
|
|
Motor axonal |
Multifocal
acquired motor axonopathy (MAMA) |
|
|
|
|
Sensory axonal |
Wartenberg
migrant sensory neuropathy Sensory
perineuritis |
|
|
|
Plexopathies
|
||||
|
Brachial |
Immune brachial
plexus neuropathy (neuralgic amyotrophy) Hereditary
neuralgia amyotrophy HNPP Thoracic Outlet
syndrome Diabetic Trauma |
|
|
|
|
Lumbosacral |
Diabetic Retroperitneal
haematoma Psoas abscess Perioperative (hip
or obstetric surgery) |
|
|
|
|
Either |
Neoplasm Radiation Infection
(Lyme, herpes, ehrlichiosis) Immune
(Sarcoid, CTDs) Vasculitiss Toxic (heroin) Amyloidosis |
|
|
|
Polyradiculopathies
|
||||
|
Inflammatory/Infectious |
Lyme Herpes zoster EBV HIV Sarcoidosis Diabetic
radiculoplexus neuropathy CISP CTDs |
|
|
|
|
Structural/ischaemic |
Spinal stenosis Large herniated
disc Arachnoiditis Epidural
lipomatosis Radiation Dural AVM Meningeaal
carcinomatosis Neoplasms NF |
|
|
|
Polyneuropathy and Optic Neuropathy
|
||||
|
|
·
B12 ·
Copper
def ·
Thiamine
def ·
Tobacco-alcohol
amblyopia ·
Cyanide ·
Hereditary o
CMT2,
HMNS-VI, LHON ·
Toxic:
Amiodarone, chloramphenicol, chloroquine, disulfiram, ethambutol, isoniazid,
linezolid, penicillamine, vincristine |
|
|
|
Myeloneuropathies (Combined Myelopathy and Polyneuropathy)
|
||||
|
|
Vitamins ·
B12,
copper, vitamin E, folate Toxic ·
Nitrous
oxide, organophosphates Inflammatory ·
CTD Infections ·
HTLV1,
HIV, Lyme Hereditary ·
Adrenomyeloneuropathy,
HSP subtypes ·
CMT2A/HMSN-V,
CMT2H, CMT2D, SCA subtypes |
|
|
|
Neuromyopathies (Combined Myopathy and polyneuropathy)
|
||||
|
|
·
Uraemia ·
Sarcoid ·
Amyloidosis ·
Paraneoplastic ·
CTD ·
Acromegaly ·
HIV,
HTLV1, Lyme ·
Critical
illness myopathy, neuropathy ·
Mitochondrial
disorders ·
Inclusion
body myositis ·
Adult
polyglucosan body disease ·
Toxic:
colchicine, chloroquine, amiodarone, L-tryptophan, vincristine |
|
|
|
Mononeuroapthy
• Numerous individual nerve syndromes (see Mononeuropathies)
Mononeuropathy
(Mononeuritis) Multiplex
• Multifocal
involvement of multiple individual peripheral nerves
• If the cause is inflammatory the term mononeuritis is used
• Vasculitis is a common cause
• Acute
o DM
o Vasculitis
• Chronic
o Multiple compressive neuroapthies
o Sarcoidosis
o Acromegaly
o Leprosy
o Lyme disease
o Carcinoma
o Idiopathic
Polyneuropathies
- Widespread,
symmetric dysfunction of the peripheral nerves
Causes
• Diabetic
• Toxic
• Nutritional
• Infections
• Inherited
• Neoplastic
• Critical illness neuropathy
OR AD VINDICATES:
• Alcohol
• Diabetes
• Vitamins (B12, B6, B1)
• Infections (HIV, leprosy)
• Neoplastic (MM, carcinoma)
• Drugs - inc. chemotherapy (Cisplatin, thalidomide)
• Inherited (CMT)
• CIDP/ Critical Illness/ CLD
• Amyloidosis (and Autoimmune)
• Toxic (Uraemia, heavy metals (lead))
• Endocrine (Hypothyroidism, acromegaly)
• Sarcoidosis
DRUGS (see below)
C4 T(o) B(low) up CAP
·
Chemotherapy
1.
Platinums
2.
Vincristine
3.
Taxanes
4.
Thalidomide
·
TB meds
o
Ethambutol
o
Isoniazid
·
Colchicine
·
Amiodarone
·
Phyenytoin
Diabetic neuropathies (see complications of DM)
Toxic
neuropathies
• Axonopathy
o Toxins
- Lead
- Mercury
o Drugs
- Colchicine
- Dapsone (motor)
- Ethambutol
- Isoniazid
- Pyridoxine
- Taxol
- Thalidomide
- Vincristine
- Bortezomib
• Myelinopathy
o Amiodarone
o Perhexiline
• Sensory Neuronopathy
o Platinum compounds
o Taxol
Nutritional Neuropathies
• Thiamine
• Pyridoxine
• Vitamin B12
• Vitamin E
Infections
• HIV
• HIV treatment
• Lymre disease
• Herpes
• Leprous neuritis
Inherited
Charcot-Marie-Tooth Disease
• Also called
• Hereditary Motor and Sensory Neuropathy
• (Peroneal muscular atrophy )
• Chronic distal sensory and motor neuropathy
• Most common heritable neuromuscular disorder (10 to 40/100,000 or 1/2500)
• Caused by mutations in >24 specific genes each with a specific phenotype
• Most genes are involved in Schwann cell function or myelination
• Generally early age of onset up to 20 years (however subtypes present later)
• Mostly AD transmission
CMT Type 1
• Demyelinating
• 5 types (CMT1A – CMT1E) based on genetics
• Type 1A most common (70-80%)– due to duplication of PMP22 gene
Clinical
• Onset often first or second decade
• Slowly progressive weakness, wasting and sensory impairment, predominantly involving the distal legs
• Weakness of – intrinsic foot, peroneal and anterior tibial
• Foot deformities (due to imbalance between intrinsic and long extensors):
o Hammer toes
o High arched feet (pes cavus)
• Loss of ankle reflexes in all patients (knee and upper limb reflexes variably involved)
• In 2/3 patients the upper limbs become involved in later life
• Palpably enlarged nerves in 25%
• Mild Kyphosis in 10%
• Can be significant worsening during pregnancy (?Effect of progesterone)
• Some patients have an upper limb tremor (Roussy-Levy Syndrome)
·
Type 2 -
(30%) – largely axonal
Investigations
• NCS
• Slow CV in all nerves (<75% of LLN)
• Slowing in upper extremities in most cases – CV <38m/s
• CMT1A CV usually 20-25ms
• CMT1B CV usually 15ms/ or less
• Generally low or absent SNAPs
• Biopsy
• Hypertrophic neuropathy - onion bulb formation, increased frequency of fibers with demyelinated and remyelinated segments, an increase in endoneurial area, and loss of large myelinated fibers
DDX:
CIDP – is a major differential diagnosis – factors that help differentiate include asymmetric pattern and raised protein in CSF
Prognosis/Natural history
• Most slowing evolves during first 3-5 years and then minimal change
• The degree of slowing has poor correlation with disability
CMT Type 2
Axonal injury
Clinical features
• Later onset than type 1 – usually teenage years – but can be later into middle life.
• Similar to type 1 however in general less severe.
• 20% of patients with mutations are asymptomatic
Investigations
Biopsy
• preferential loss of large myelinated fibers, without
significant demyelination
Other types of CMT
X-Linked CMT (CMTX)
7-16% of CMT
Similar to CMT1
Males severely affected
Female carriers often have very mild disease
Need to caution about travelling to high altitude as has been associated
with worsening
CMT Type 3
Rare
Most cases are sporadic, some AR
Severe neuropathy often associated with severe weakness and
disability.
Severe slowing and demyelination
High CSF protein
CMT Type 4
Multiple forms, all autosomal recessive
Onset in early childhood
Often associated with other congenital abnormalities
Severe slowing consistent with demyelination
Clinical features
·
Wasting and weakness of the distal muscles of the
legs (inverted champagne bottle legs)
·
Deformities
o
Hammer toes
o
High arched feet (pes cavus)
·
Distal sensory loss
o
Both pain and vibration sense
o
Often mild with minimal symptoms
·
Loss of reflexes
o
Universally at ankles and to a lesser extent
elsewhere
·
Tremor may occur in 10%
Investigations
Nerve conduction studies
·
Type I
o
Decreased velocities in both motor and sensory
·
Type II
o
Velocities are near normal
Nerve biopsy- sural nerve
·
Can help confirm diagnosis
CSF
·
May be helpful to help exclude CIDP which is major
differential
Management
Ascorbic acid and anti-progesterones have been trialled but were not
effective.
Avoid worsening of neuropathy
Avoid medications that can cause neuropathy
Moderate alcohol
Prompt treatment of diabetes
Physiotherapy
Strengthening, posture and balance excercises
Orthoses to support foot
Pain management
Neuropathic pain management
Treat resultant joint and muscle pain
Surgical treatment
Osteotomy, arthrodesis, plantar fascia release
Genetic counselling
Hereditary Neuropathy with Liability to
Pressure Palsy
·
A form of CMT disease
·
Recurrent episodes of focal entrapment neuropathy
·
Peroneal, ulnar, radial and median
·
Associated with specific genetic abnormality